An artificial pancreas system—also called a bionic pancreas, closed-loop system, or automated insulin delivery system—is a set of components that work together to imitate the blood glucose-controlling action of a healthy pancreas.
Artificial pancreas systems are mainly used to regulate blood glucose (sugar) levels in people with type 1 diabetes.
In type 1 diabetes, the natural pancreas produces little insulin or none at all. To maintain a healthy range of blood glucose levels, people living with the condition must regularly monitor their blood glucose, calculate how much insulin they need, and then administer it. Artificial pancreas systems automatically perform these functions throughout the day and night. Healthy blood glucose levels reduce the risk of developing diabetes-associated complications.
Artificial pancreas systems greatly simplify blood sugar control, but they are not entirely hands-off. They still require effort from the user in the form of carbohydrate counting and adjusting settings to help determine how much insulin is adequate. This is why they are called hybrid closed-loop systems.
How do artificial pancreas systems work?
Different systems look and feel different, but they all have 3 basic components which enable them to do their work. These components are:
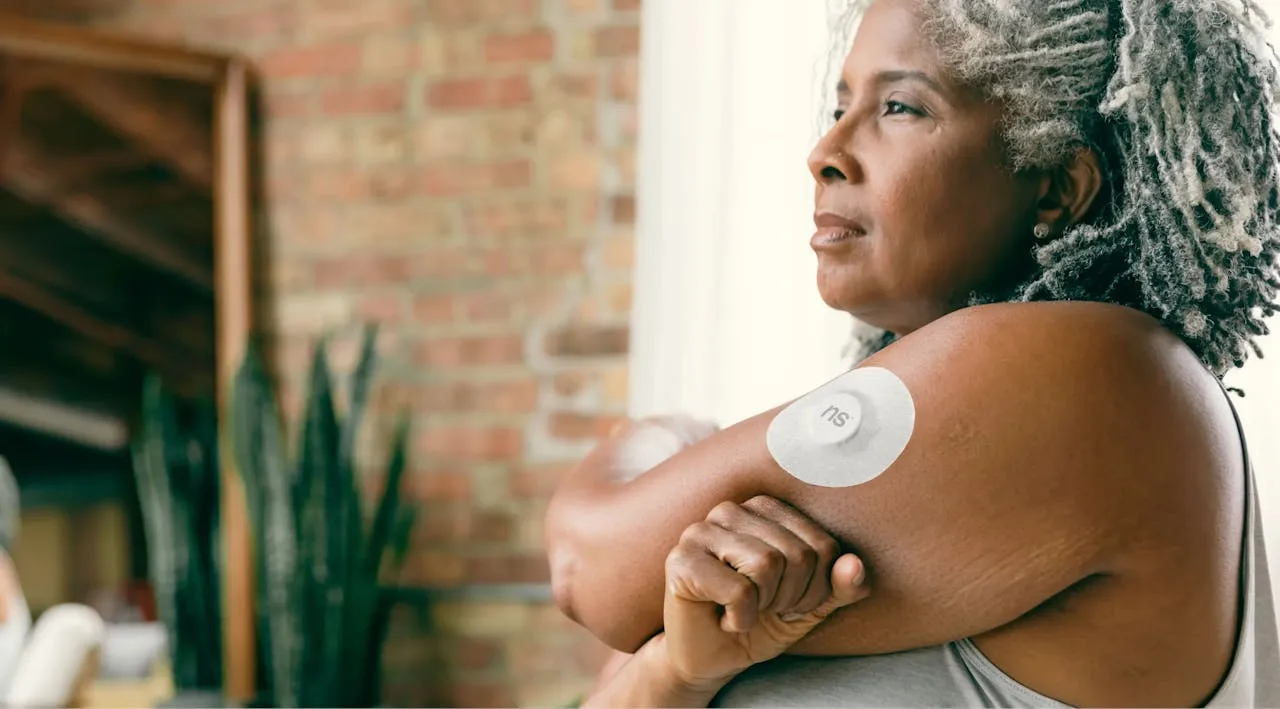
A continuous glucose monitor (CGM)
A CGM consists of a small sensor under the skin that measures glucose levels. A transmitter wirelessly sends information from the sensor to a program on an insulin pump or a smartphone. Adhesive tape is used to keep the sensor and transmitter in position.
Control algorithm
This is a software program that receives glucose information from the sensor, performs a series of calculations, and determines how much insulin is needed to control blood glucose levels. It then sends dosing instructions to the insulin pump.
Insulin pump
Basing on the dosing instructions, the pump will automatically deliver insulin under the skin.
Some insulin pumps are fitted onto a belt, kept in a pocket, or a pouch. So, insulin is delivered through a thin plastic tube that connects the pump to a smaller, flexible tube under the skin. Other insulin pumps are attached directly to the skin with an adhesive patch. They have no external tube, but insulin is delivered by a thin plastic tube under the skin.
What are the types of artificial pancreas systems?
The systems can be classified into 2 types, depending on how many hormones they release. The types are:
I. Insulin-only systems
They continuously monitor blood glucose levels and regulate them by automatically increasing or decreasing how much insulin they deliver to your body.
II. Dual-hormone systems
Glucagon is another hormone produced by a healthy pancreas. Unlike insulin, glucagon raises blood glucose levels.
Dual-hormone systems mimic a healthy pancreas better by using synthetic glucagon and insulin to closely control blood glucose levels without causing hypoglycemia. Hypoglycemia is when your blood glucose levels are lower than normal. It is a serious complication of insulin therapy that can cause dizziness, anxiety, sweating, blurry vision, seizures, and coma.
Other dual hormone systems in development combine delivery of insulin and pramlintide, a medication which controls post-meal blood glucose levels by decreasing glucagon secretion and slowing emptying of food from your stomach.
Artificial pancreas systems can also be classified into 2 types, depending on how they prevent hypoglycemia. The systems can be:
- Threshold suspend systems: These systems monitor blood glucose levels and automatically stop administering insulin when levels drop to a certain pre-set level.
- Predictive low-glucose suspend systems: These systems use measured glucose levels and algorithms to predict a decline in glucose levels. They stop delivering insulin before blood glucose gets too low.
Who can use artificial pancreas systems?
Doctors usually prescribe the systems for people with type 1 diabetes. They can be used by adults and children older than 2 years. Your doctor will help with determining what system is best for you, and a diabetes educator will train you on how to use it.
Other than simplifying blood sugar control in people with type 1 diabetes, a doctor might also prescribe an artificial pancreas system if you:
- Have insulin-dependent type 2 diabetes.
- Have had your pancreas surgically removed.
- Have cystic fibrosis-related diabetes. Cystic fibrosis is a genetic disorder that can cause thickening of secretions in the pancreas and eventually decreased insulin production.
What are the benefits of artificial pancreas systems in managing diabetes?
Artificial pancreas systems ease the management of diabetes and improve the quality of life for people living with the condition and those who care for them. Benefits of using the systems include:
- Keeping your blood sugar within target range and preventing episodes of hypoglycemia and hyperglycemia (high blood glucose).
- Making personalized diabetes care easier. Besides automatically adjusting insulin depending on your own glucose levels, glucose data can be shared with your diabetes care team. Your doctor can then recommend further dosage adjustments if necessary.
- Reducing the need for finger stick glucose tests.
- Reducing your chances of getting long-term diabetes-related complications like nerve damage, eye disease, kidney disease, and heart disease.
- Improving quality of sleep in people with diabetes and those who care for them.
- Relieving the anxiety of managing diabetes manually.
What are the limitations of artificial pancreas systems?
Like any other helpful technology, artificial pancreas systems still present some challenges to those who use them. Some common limitations of these systems include:
- You always have to wear the devices on your body. This can be uncomfortable for a lot of people and may even interfere with physical activity.
- The adhesive tape used to hold the components in position may cause skin redness, itching, rash, and bruising.
- At the site where the insulin pump delivers insulin, you might notice nodules under the skin due to fat accumulation. Rarely, loss of fat under the skin can happen and this will appear as skin indentation.
- Purchasing these systems and regularly replacing their supplies may be expensive for some people.
- The systems may not always be accurate. Compression of the sensor and medications like paracetamol, aspirin, hydroxyurea, and vitamin C supplements can interfere with the accuracy of the glucose monitor. Malfunctioning of system components can also affect glucose monitoring and insulin delivery.
- These systems still require user input and using them may seem complicated, especially after just after getting them. Luckily, your team will guide on how to get started with using them. A healthcare provider will train you on how to:
- Calibrate the CGM whenever necessary, identify sensor issues, interpret CGM information, insert and replace CGM sensors.
- Count the amount of carbohydrates in your meals and enter them in the system.
- Make sure the insulin pump works well. You will also learn how to identify problems with the insulin delivery set and how to connect and disconnect the delivery set.
- Adjust the settings of the computer program.
What are DIY artificial pancreas systems?
Do-It-Yourself (DIY) artificial pancreas systems are those which use open-source algorithms, commercially available CGMs and insulin pumps to monitor and regulate blood glucose. They are also called open-source artificial pancreas systems.
The algorithms are developed and modified by individuals in a collaborative online community, typically people with diabetes or their relatives. The algorithms are freely available on the internet, so DIY systems offer a cheap alternative to FDA approved systems.
DIY systems are unregulated, so healthcare professionals can’t prescribe them and most have limited knowledge on how the systems work. But most professionals should still offer support and guidance to help control your diabetes even if you’re using these systems.
DIY systems require technical skills to build and maintain, but they don’t come with user manuals, so you should always have a back-up plan in case any component fails.
The future of artificial pancreas technology
As the systems become more widespread and funding for research and development increases, they are likely to become more efficient and easier to use. Some exciting features and capabilities being explored include:
- Better artificial pancreas hardware. There are efforts to improve the shape, battery life, size, and longevity of system components.
- Fully automated systems that don’t require carbohydrate counting and manually changing modes.
- Dual-hormone systems that combine delivery of insulin and glucagon, pramlintide, or glucagon-like peptide-1 (GLP-1) receptor analogs. GLP-1 receptor analogs are medications used to manage obesity and type 2 diabetes.
- Intraperitoneal insulin delivery. This is where insulin is administered in the space between the 2 layers that line the abdomen. This offers better after-meal blood glucose control than administration of insulin under the skin.
- Use of artificial intelligence to improve user experience and to make blood glucose control better.
Are there natural alternatives to artificial pancreas systems?
Yes, pancreas and islet cell transplantation are medical procedures that can restore the body’s ability to produce insulin.
Pancreas transplantation is where an entire damaged pancreas is replaced by a healthy one from a donor. It is a risky procedure that is typically reserved for people who also have advanced kidney disease and need a simultaneous kidney transplant.
Pancreatic islet cells are the hormone making cells of your pancreas. Insulin is produced by the beta cells and glucagon is produced by the alpha cells. Beta cells are the most abundant type of islet cells. Islet cell transplantation involves transferring healthy islet cells into the liver of a person with diabetes.
After any of these procedures, you will need lifelong immunosuppressive medications and these can have serious side effects.
The takeaway
Artificial pancreas systems represent a significant step forward in diabetes management. These systems reduce the burden of constant monitoring and injections. By mimicking the body’s natural insulin regulation, they help maintain more stable glucose levels, improving overall health and quality of life.
While not yet a cure, artificial pancreas systems offer hope for people living with diabetes. As technology continues to evolve, they are becoming more accurate and accessible. If you or a loved one could benefit, talk to your healthcare provider about whether these systems are right for you.