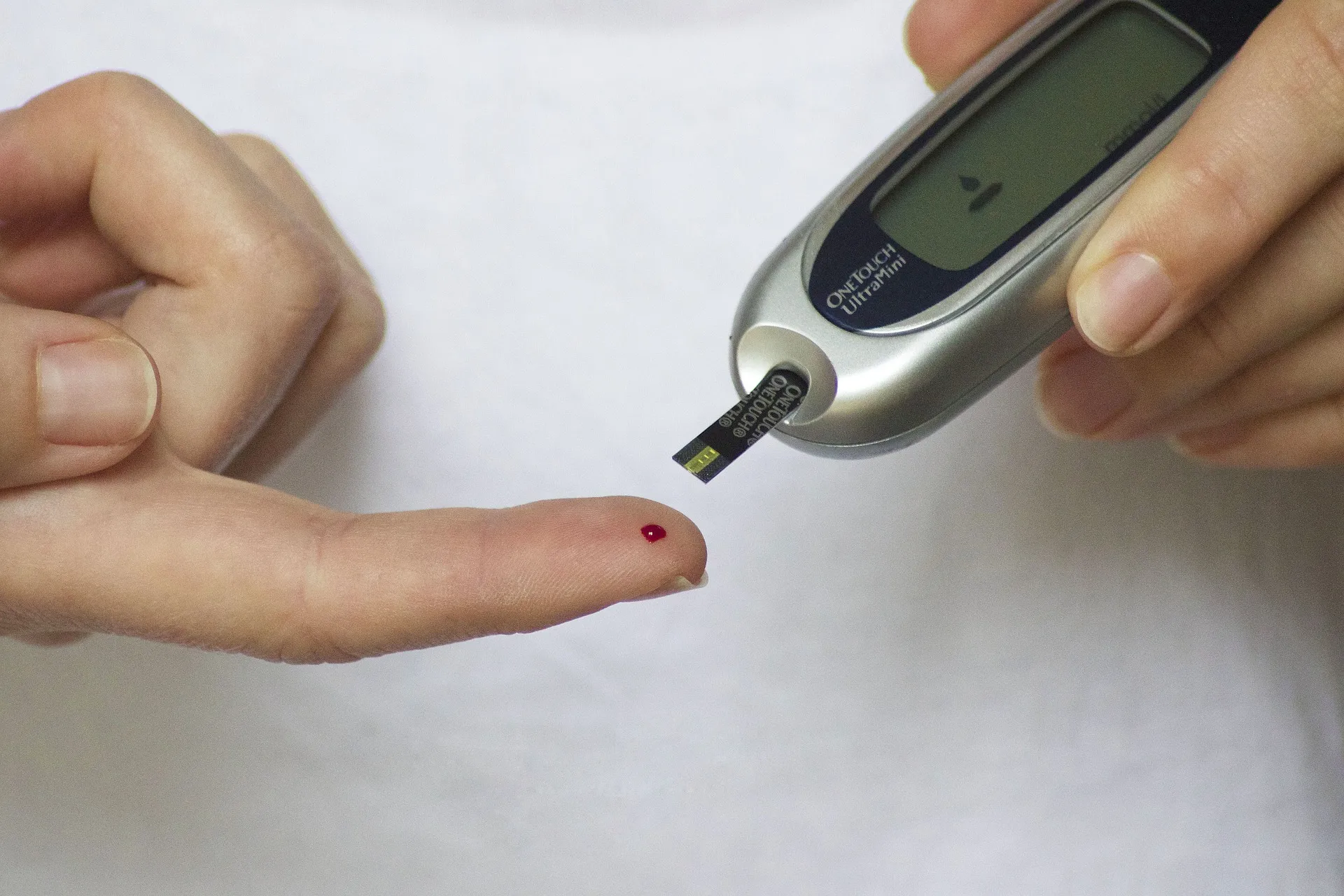
Hypoglycemia, also called low blood sugar or low blood glucose, is a condition where your blood sugar (glucose) falls below a level that is healthy for you.
The blood sugar cut-off for hypoglycemia is different in those with diabetes from those without it. If you have diabetes, hypoglycemia is when you have blood sugar less than 70 milligrams per deciliter (mg/dL) or 3.9 millimoles per liter (mmol/L).
For those without diabetes, hypoglycemia is typically when someone’s blood sugar is less than 55 mg/dL or 3.1 mmol/L.
Low blood sugar is more common in diabetic people taking certain diabetes medications. Those with type 1 diabetes also experience hypoglycemia more often than those with type 2 diabetes.
What causes hypoglycemia?
Glucose is the main source of energy for your body’s cells. Blood glucose (sugar) mainly comes from consumption of carbohydrate-rich foods and drinks.
Two hormones from your pancreas (a gland in your abdomen behind the stomach) are the major regulators of your blood sugar. They are: insulin and glucagon. After a meal, insulin reduces blood sugar by allowing your body’s cells to take it up from the blood. Glucagon is produced when you have low blood sugar. It mobilizes glucose from stores in your liver.
Anything that alters the balance of the blood sugar-regulating hormones or how the body processes glucose can cause hypoglycemia.
Causes of diabetes-related hypoglycemia
Some common causes of low blood sugar in people with diabetes include:
- Taking too much insulin
- Injecting insulin into muscle instead of the fat tissue under the skin. Intramuscular insulin is absorbed very fast and can cause a rapid fall in blood sugar.
- Taking high doses of oral anti-diabetes medicines, especially sulfonylureas and meglitinides.
- Skipping meals, eating less food than usual, or eating later than usual but taking diabetes medications at the usual time.
- Taking alcohol without eating. Alcohol blocks gluconeogenesis, the process by which cells in the liver and kidneys form new glucose.
Causes of non-diabetic hypoglycemia
Non-diabetic (spontaneous) hypoglycemia is an uncommon condition. There are 2 major types of hypoglycemia that can affect anyone, including those without diabetes. These types have different causes, and they are:
I. Reactive (postprandial) hypoglycemia
This is where your blood sugar falls to lower than normal after a meal or snack. It typically happens within 4 hours after eating. It may be caused by:
- Consuming foods rich in simple carbohydrates like potatoes, white bread, white rice, pastries, and white pasta.
- Bariatric surgery (weight loss surgery)
- Glycogen storage diseases. These are conditions that affect how the body uses glycogen, the storage form of glucose.
II. Fasting hypoglycemia
During periods of fasting, hormones such as glucagon, growth hormone, cortisol, and adrenaline are released to help maintain normal blood sugar levels. These hormones stimulate gluconeogenesis and cause your body to break down stored glycogen. So, fasting usually doesn’t cause hypoglycemia in most people.
When hypoglycemia happens after a period of not eating food, it may be due to:
- Critical illnesses like end-stage liver disease, sepsis, starvation, severe malaria, or kidney failure. When you have these conditions, your body may use up more glucose than you consume, and faster than your body can create new glucose.
- Some non-diabetes medications like beta-blockers, certain antibiotics, quinine, pentamidine, and angiotensin-converting enzyme inhibitors.
- Excessive alcohol intake.
- Adrenal insufficiency. This is where your adrenals do not produce enough cortisol.
- Growth hormone deficiency.
- An insulinoma. This is a rare tumor in the pancreas that releases too much insulin, leading to low blood sugar.
- A non-islet cell tumor. Non-islet cell tumors produce excess insulin-like growth factor 2 (IGF-2). IGF-2 is a hormone that mimics the actions of insulin.
What are the symptoms of hypoglycemia?
When your blood sugar falls below a healthy level, your symptoms might include:
- Sweating
- Trembling
- Hunger
- Anxiety
- Fast, irregular, pounding heart beat
- Inability to concentrate
- Irritability and anger
- Drowsiness and fatigue
- Pale skin
- Confusion
- Nausea
- Headache
- Blurry vision
- Abnormal behavior
- Slurred speech
- Loss of coordination
- Loss of consciousness
- Seizures
Nocturnal hypoglycemia is where you develop low blood sugar during sleep. Symptoms of this condition include:
- Early morning headaches
- Unpleasant dreams
- Excessive sweating during the night
- Crying out during sleep
- Feeling tired or irritable after waking up
What is hypoglycemia unawareness?
This condition, also called impaired hypoglycemia awareness or hypoglycemia-associated autonomic failure, is where people with long-standing diabetes or recurrent hypoglycemia do not experience the symptoms of hypoglycemia.
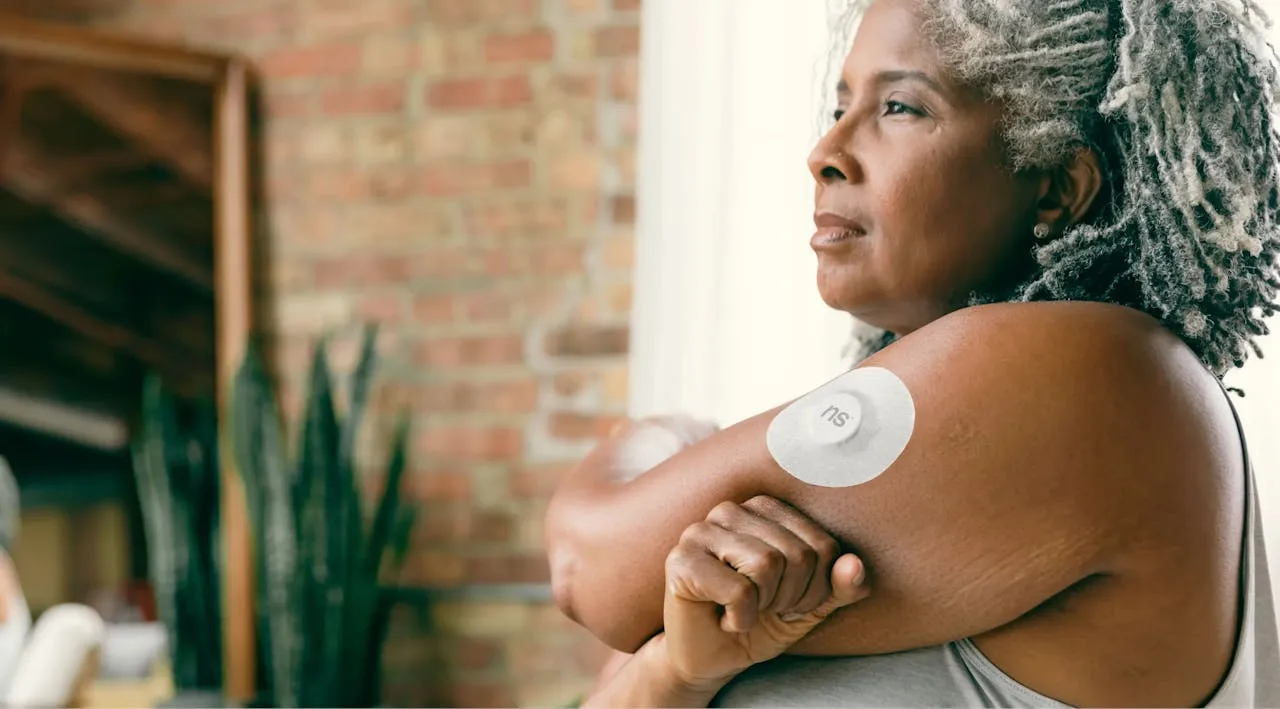
You are at a high risk of getting severe episodes of hypoglycemia if you have this condition. Having it will require you to monitor your blood sugar closely. You might need to use a continuous glucose monitor (CGM) for this. More frequent manual glucose tests and diabetes alert dogs may also help you to identify falling blood sugar before it gets dangerously low.
If you don’t experience hypoglycemia symptoms despite having low blood sugar readings, seek medical attention immediately.
How is hypoglycemia diagnosed?
If you have diabetes, it is essential to check your blood sugar with a glucose meter (glucometer) as soon as you experience symptoms of hypoglycemia. If you are currently using a CGM to monitor your blood sugar, it should be able to warn you if your blood sugar is tending toward hypoglycemia or is already below the lower limit of a preset range.
When you have diabetes and symptoms of low blood sugar but have no glucometer or CGM, your symptoms are enough to diagnose hypoglycemia.
If you don’t have diabetes but have symptoms of hypoglycemia, seek medical help as soon as you can. In the hospital, a doctor will confirm the condition by checking if you meet the 3 criteria which make up the Whipple’s triad. The criteria are:
- Signs and symptoms of low blood sugar. The doctor will ask you about your symptoms, their timing, and what medications you are taking.
- Evidence of low blood sugar at the time of the symptoms. You will have a blood sample taken, and your blood sugar measured in a laboratory.
- Resolution of the hypoglycemia signs and symptoms after increasing your blood sugar.
Your doctor might also order for additional tests to identify the cause of your hypoglycemia. Some of these tests are:
- Kidney function tests
- Liver function tests
- Blood levels of insulin and C-peptide―a protein produced by the pancreas alongside insulin.
- Early morning cortisol levels
- Imaging tests such as computed tomography (CT) scans and magnetic resonance imaging (MRI) scans to check for tumors.
How is hypoglycemia treated?
If your blood sugar is lower than 70 mg/dL, or you have symptoms of hypoglycemia but are unable to check your blood sugar level, you need to raise your blood sugar as soon as possible by consuming a carbohydrate-rich food or drink.
You can use the 15-15 rule to treat an episode of hypoglycemia. You do this by:
- Eating or drinking 15 grams (g) of glucose or fast-acting carbohydrate.
- Wait for 15 minutes then check your blood sugar. If it’s still below 70 mg/dL, consume another 15 g of glucose or fast-acting carb.
- After 15 minutes, check your blood sugar again.
- Repeat these steps until your blood sugar rises above 70 mg/dL. Once it’s above that, have a protein and carbohydrate snack to keep it from dropping again.
Examples of foods that contain about 15 g of fast-acting carbs include:
- 1 tablespoon of sugar, honey, or corn syrup.
- A half can (4–6 ounces) of regular soda, not diet soda.
- A half cup (4 ounces) of regular fruit juice.
- Hard candies or jellybeans. Check the nutrition label to find out how many contain 15 g of carbs.
- 3–4 glucose tablets or one packet of glucose gel.
If someone with hypoglycemia is unwilling to take carbs orally, has slurred speech, is disoriented, has seizures, or is unconscious, they need to receive synthetic glucagon. It works just like the glucagon produced by the pancreas. Synthetic glucagon can be administered as a nasal spray or an injection.
Anyone can administer glucagon. If you’re having trouble using a glucagon kit, check the instructions on the package.
In the hospital, medications that the doctor may use to raise your blood sugar include:
- Synthetic glucagon
- Dextrose, a type of sugar that is chemically similar to glucose.
- Octreotide (Sandostatin)
- Diazoxide (Proglycem)
What are the complications of hypoglycemia?
Mild or moderate hypoglycemia usually doesn’t cause serious issues. But severe prolonged hypoglycemia can be life-threatening.
Glucose is the primary source of energy for the brain. And unlike other organs, the brain stores very little glucose so it depends on a steady supply of glucose in the blood to keep functioning. Thus, most complications of hypoglycemia are due to disrupted supply of glucose to the brain.
Complications of low blood sugar include:
- Seizures
- Permanent brain damage
- Abnormal heart beats (cardiac arrhythmias)
- Cardiac arrest
- Multi-organ failure
- Coma
- Death
How can hypoglycemia be prevented?
Preventing hypoglycemia may not always be simple for people who have diabetes or any other condition that causes low blood sugar. But it is possible.
Steps you can take to prevent your blood sugar from falling below a healthy level include:
- Constantly tracking your blood sugar levels with a continuous glucose monitor (CGM). A CGM can help you and your diabetes care team to identify patterns and triggers of hypoglycemic episodes. It also allows you to take action early if your glucose is trending toward hypoglycemia.
- Following the doctor’s or pharmacist’s instructions on the amount, timing, and administration method of your diabetes medications.
- Taking to a dietitian to help you develop a diet plan that is compatible with your diabetes treatment plan.
- Having safe exercise habits. You need to be consistent with the timing and intensity of your exercise. You may also need to monitor your blood sugar before, during, and after physical activity to make sure you adjust your snacking and medication schedule as necessary to prevent hypoglycemia.
- Finding help to reduce your alcohol intake, if you have alcohol use disorder. This is especially helpful if you take insulin to manage your diabetes. Whenever you take alcohol, make sure you eat food at around the same time.
Frequently asked questions
How can I prepare for episodes of hypoglycemia?
It may not be entirely possible to prevent your blood sugar levels from falling too low. If you have recurrent hypoglycemia or are at high risk of getting low blood sugar, you might benefit from having a plan to have it promptly treated when it develops. You can stay prepared by:
- Wearing medical alert identification like a bracelet or necklace. It lets people know that you have diabetes and enables them to offer appropriate care in case of an emergency.
- Always have an emergency glucagon kit. Check its expiry date regularly and make sure you replace it before this date. You may need to ask a certified diabetes care and education specialist (CDCES) to teach you how to use it. If that’s not possible, you can watch a YouTube video on how to use it.
- Whenever you leave home, carry sources of fast-acting carbs, such as glucose gel packets, juice boxes, hard candy, and glucose tablets.
- Teach your relatives, coworkers, roommates, or teachers about hypoglycemia, how it is treated, and tell them where they can find your emergency hypoglycemia treatment kit.
What is the difference between hyperglycemia and hypoglycemia?
“Hyper-” means “above” and “hypo-” means “below”. Hyperglycemia means blood sugar above the healthy range and hypoglycemia means blood sugar below the healthy range.
What is pseudo-hypoglycemia?
This is where some people with diabetes have symptoms of hypoglycemia even when their blood sugar is higher than the lower limit of a healthy blood sugar range. It happens in people with long-standing diabetes because chronic high blood sugar (hyperglycemia) raises the “set-point” at which symptoms of low blood sugar appear.
What should I remember?
Hypoglycemia, though often associated with diabetes, can occur in people without the condition. Causes include excessive alcohol consumption, certain medications, critical illnesses, or hormonal imbalances. Recognizing symptoms like shakiness, confusion, and sweating is crucial to act quickly.
If you suspect hypoglycemia, consume a fast-acting carbohydrate, such as juice or glucose tablets, and seek medical advice to identify the underlying cause. Understanding and managing this condition can prevent complications and improve quality of life. Always consult a healthcare provider for personalized guidance.