Resistant hypertension refers to blood pressure that remains above someone’s target goal despite treatment with maximally tolerated doses of three or more blood pressure medications, one of which is a diuretic. If your blood pressure is only controlled by taking 4 or more antihypertensive medications, you will also be diagnosed with resistant hypertension.
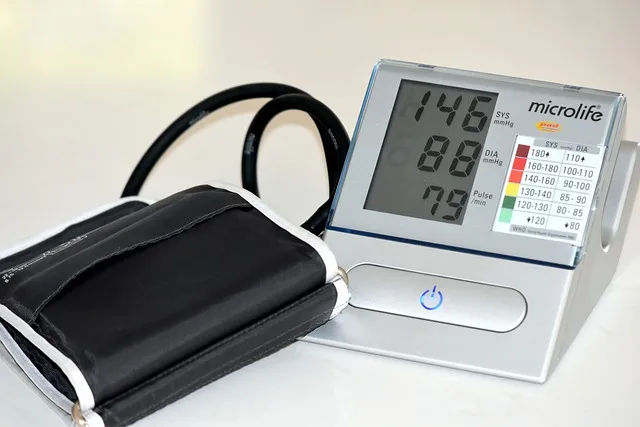
For most people in the U.S., the goal of treatment is blood pressure less than 130/80 millimeters of mercury (mmHg). In most of the other countries outside the U.S., the goal for most people is blood pressure less than 140/90 mmHg.
Worldwide, about 1 in 10 people taking blood pressure medications has resistant hypertension. In people with chronic kidney disease and high blood pressure, resistant hypertension affects about 2 in 10 of them taking antihypertensive medications.
Uncontrolled or poorly controlled high blood pressure is a serious condition that increases your risk of getting serious health complications.
What causes resistant hypertension?
While most cases of resistant hypertension have no known medical cause, some of them result from identifiable (secondary) medical causes. High blood pressure that is caused by an underlying medical condition or medication is called secondary hypertension.
Secondary causes of resistant hypertension include:
I. Medical conditions
To ensure blood pressure control, these conditions need to be identified and treated. They include:
- Renal artery stenosis. This is narrowing of the arteries to your kidneys.
- Chronic kidney disease
- Narrowing (coarctation) of the aorta
- Obstructive sleep apnea
- Acromegaly, a condition of excess growth hormone production during adulthood.
- Thyroid disorders
- Disorders where your adrenal glands produce an excess of certain hormones that increase blood pressure. Examples are:
- Primary aldosteronism, where there is too much aldosterone hormone.
- Cushing’s syndrome, where there is too much cortisol hormone.
- Phaechromocytoma. This is a rare tumor that produces too much adrenaline and noradrenaline.
II. Drugs and medications
Medications and drugs that can make your blood pressure unresponsive to treatment include:
- Birth control pills (oral contraceptives)
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Nasal decongestants
- Corticosteroids like dexamethasone and prednisolone
- Stimulants like cocaine, amphetamine, and methamphetamine
- Licorice
What are the symptoms of resistant hypertension?
Many people with hypertension do not know that they have the condition. That’s because you can have it without having symptoms. But when it is not treated, it can rise to dangerous levels and cause symptoms like:
- Shortness of breath
- Headache
- Chest pain
- Nosebleeds
- Blurry vision
What are the risk factors of resistant hypertension?
These factors contribute to high blood pressure and make it harder to control, but don’t directly cause it. They include:
- Having diabetes
- Having obesity
- Excessive salt intake
- Taking too much alcohol
- Being physically inactive
- Being black
- Old age
- Male sex
- Being chronically stressed
What is pseudo-resistant hypertension?
Pseudo-resistant hypertension is high blood pressure that appears unresponsive to treatment due to factors interfering with treatment and blood pressure measurement. It mimics true resistant hypertension but becomes well controlled when these factors are addressed.
Common causes of pseudo-resistant hypertension include:
- Inaccurate blood pressure measurement. This can be due to improper technique or using the wrong size of arm cuff.
- Non-adherence to blood pressure medications.
- White-coat hypertension. This where your blood pressure is high in the hospital but normal at home.
- Stiffening of the brachial artery―a blood vessel in the upper arm around which arm cuffs are placed during measurement of blood pressure.
How is resistant hypertension diagnosed?
A doctor will start with taking your full medical history. This involves telling them about any symptoms you have, how long you have had hypertension, what supplements and drugs (prescription, recreational, herbal, and over-the-counter) you are currently taking, and how often you take them.
A healthcare worker will then use an appropriately sized arm cuff to measure your blood pressure. To rule out white-coat hypertension, your doctor might suggest home blood pressure measurement or 24-hour ambulatory blood pressure monitoring (where your blood pressure is measured and recorded throughout the day).
You might also be screened for secondary hypertension. To check for its causes, tests that may be done include:
- Urine analysis to check for kidney damage.
- Blood tests for the levels of thyroid and adrenal glands hormones.
- Sleep study to check for obstructive sleep apnea.
- Echocardiography (Echo) to check for coarctation of the aorta.
- Ultrasound scanning, computed tomography (CT) scanning, and magnetic resonance imaging (MRI) to check for problems with the kidneys or renal arteries.
How is resistant hypertension treated?
Treatment of resistant hypertension mainly involves taking antihypertensive medications and modification of lifestyle factors that contribute to the development of the condition. Treatment strategies include:
Lifestyle changes
Modifications that you might be required to make include:
- Exercising regularly.
- Dietary changes. Blood pressure-reducing changes you can make to your diet involve limiting daily sodium intake to no more than 2,300 mg and following a hypertension-friendly eating pattern, for example the DASH diet.
- Attaining and maintaining a healthy weight.
- Adjusting the dose or stopping the use of blood pressure-raising medications. Do not make any changes to medications you’re taking before talking to your doctor.
- Reducing your alcohol intake.
Medications
Taking medications as directed by a doctor or pharmacist is essential for keeping high blood pressure in check.
Many people can have seemingly resistant hypertension because of non-adherence or poor adherence to their medications. This may be due to insufficient knowledge about the medications, unpleasant side effects, or a high pill burden (this is where you take many pills on a daily basis). If you have any of these issues, talking to your doctor can help you find solutions and this will enable you to achieve your treatment goals.
If you still have resistant hypertension despite taking your medications promptly, your doctor may add another medication to your treatment plan or substitute one drug for another. Common types of medications that can be used to treat resistant hypertension are:
- Calcium channel blockers
- Diuretics (water pills)
- Angiotensin receptor blockers (ARBs)
- Angiotensin-converting enzyme (ACE) inhibitors
- Beta-blockers
Renal denervation (RDN)
It is also called renal nerve ablation. It is a minimally invasive procedure where nerves in the renal arteries are destroyed. This reduces nerve activity in the kidneys, which brings down blood pressure.
What are the complications of resistant hypertension?
Untreated resistant hypertension may cause complications like:
- Stroke
- Heart failure
- Kidney disease
- Dementia
- Retinopathy. This is damage to the retina—the lining at the back of each eye which allows us to see.
How can I prevent resistant hypertension?
It may be impossible to prevent secondary causes of resistant hypertension. But, it’s possible for everyone with high blood pressure to take certain steps to prevent resistance to treatment. These steps include:
- Staying at a healthy weight.
- Taking antihypertensive medications as directed by a health worker. If you have to take any medicines alongside your blood pressure drugs, consult with your doctor first.
- Limiting salt intake.
- Cutting down or abstaining from alcohol intake.
- Getting adequate, uninterrupted sleep every night.
- Engaging in moderate-intensity exercise for at least 150 minutes every week. Find out how to use exercise to reduce blood pressure.
- Finding healthy ways to deal with stress.
What should I remember?
Resistant hypertension is high blood pressure that remains uncontrolled despite using three or more medications, including a diuretic. It increases the risk of heart disease, stroke, and kidney damage. Identifying and treating underlying causes, such as sleep apnea or hormone problems, is key to better control.
If your blood pressure stays high despite treatment, work closely with your doctor to adjust your plan. Lifestyle changes, like reducing salt, exercising, and managing stress, can help. With the right approach, resistant hypertension can be managed to protect your long-term health.