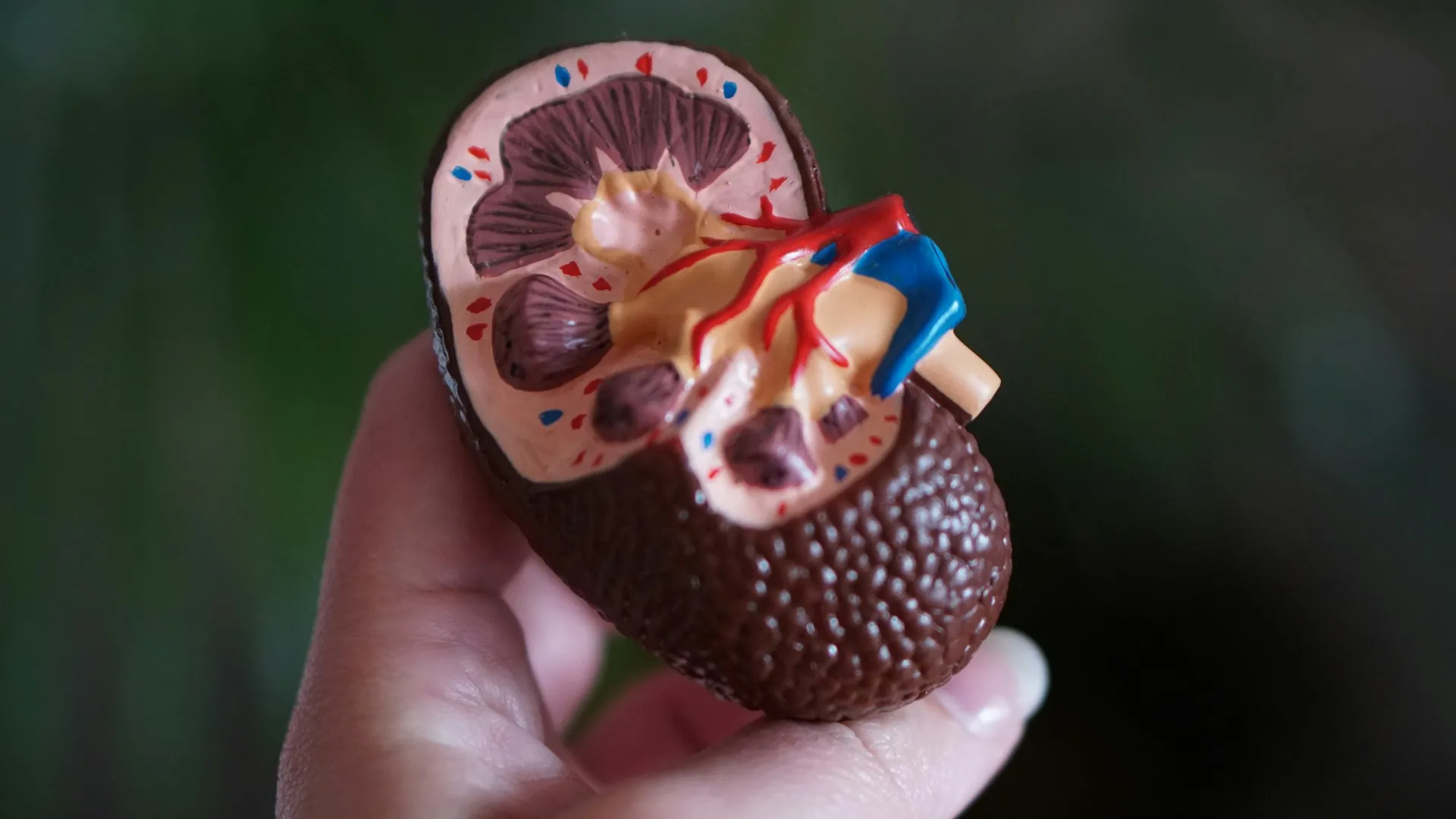
Renal hypertension, also called renovascular hypertension, is a condition where narrowing or blockage of the renal arteries causes high blood pressure.
High blood pressure (hypertension) is when the force your blood applies on the walls of your arteries is consistently too high. According to World Health Organization (WHO), you have hypertension if your blood pressure is 140/90 millimeters of mercury (mmHg) or more. According to the American College of Cardiology and American Heart Association, you are diagnosed with hypertension if your blood pressure is 130/80 mmHg or more.
There are two types of hypertension: secondary and primary (essential) hypertension, which accounts for 90% of all adult cases of high blood pressure.
Secondary hypertension is when a specific medication or condition can be identified as the cause of high blood pressure. Renal hypertension is one of the most common causes of secondary hypertension.
What causes renal hypertension?
The kidneys are 2 bean-shaped organs located in the back of your abdomen, each on one side of your spine. They perform a number of functions to make sure you stay healthy.
A renal artery branches off from either side of your aorta, each artery supplying most of the blood to the kidney on its side. Narrowing (stenosis) or blockage of these arteries can be caused by conditions such as:
- Atherosclerosis, a condition where a sticky substance called plaque builds up in your arteries. Atherosclerosis causes about 90% of all cases of renal artery stenosis.
- Fibromuscular dysplasia, a condition of abnormal growth of cells in the walls of your arteries. It causes about 9% of cases of renal hypertension.
- Inflammation of the arteries, such as in Takayasu’s arteritis.
- Renal artery dissection. This is a build up of blood within the walls of the renal arteries.
- External compression of the renal artery, which may be caused by tumors.
- Radiation fibrosis. This is accumulation of scar tissue in parts exposed to radiation therapy.
- Obstruction due to surgery on the aorta or renal arteries.
When there is reduced blood flow to your kidneys, they release an enzyme called renin. Renin activates other substances in the Renin-Angiotensin-Aldosterone System (RAAS), a system of hormones and enzymes that regulates your blood pressure and blood volume.
Angiotensin II, a hormone in the RAAS system, will then increase your blood pressure by causing vasoconstriction (narrowing of the small arteries throughout the body).
Aldosterone, another hormone in the RAAS system, causes your kidneys to retain salt and water, further increasing your blood pressure.
What are the symptoms of renal hypertension?
Renal hypertension usually has no symptoms until it is serious enough to damage your kidneys or other organs. Symptoms of severe kidney dysfunction that you may notice include:
- Unexplained weight loss
- Nausea and vomiting
- Loss of appetite
- Muscle cramps
- Swelling in the feet, hands, and face
- Generalized itchiness or numbness
- Headaches
- Trouble sleeping
- Difficulty concentrating
- Shortness of breath or chest pain
- Urinating more often, or less often than usual
Who is at risk of getting renal hypertension?
Renal hypertension can affect anyone. People who are at risk of getting atherosclerosis are more likely to get the condition. Risk factors for atherosclerosis include:
- Being older than 55 years
- Having high blood cholesterol levels
- Having a history of smoking
- Living with diabetes
- Obesity
- Sedentary lifestyle
- Having a family history of cardiovascular disease
- Consuming a diet high in saturated and trans fats
Fibromuscular dysplasia is typically seen in women under 50 years, and is believed to be familial.
How is renal hypertension diagnosed?
To diagnose this condition, a doctor will take a medical history, physically examine you, and request that you have certain tests done. As part of obtaining a history, your doctor will ask about any symptoms you have noticed, your family history, other medical conditions you have and the medicines you are taking.
Am important clue from your history that may suggest you have renal hypertension is having uncontrolled high blood pressure despite taking maximum doses of 3 or more antihypertensive medications from different classes, one of which is a diuretic.
A healthcare professional will measure your blood pressure with a blood pressure cuff, and record it. You may have your blood pressure measured more than once to confirm that you have high blood pressure.
Your doctor may also use a stethoscope on your abdomen to listen for sounds of narrowed arteries. A whooshing sound called a bruit may be heard if your renal arteries are narrowed.
Imaging tests that may be done to confirm that your renal arteries are blocked or narrowed include:
- Duplex ultrasonography: This test uses sound waves to produce images that can be used to show reduced or absent blood flow through the renal arteries. However, it may not be accurate in obese patients or when performed by a technician who is not adequately skilled.
- Magnetic Resonance Angiography (MRA): This test used strong magnetic fields and radio waves to generate images that show blood flow in your renal arteries, and the structures around the arteries. Contrast medium may be injected into your vein to help see your arteries better.
- Computed Tomography Angiography (CTA): Here, contrast medium is injected into a vein on your arm and X-rays are used to create images that show blood flow in your renal arteries.
- Catheter angiography: In this invasive test, a healthcare professional makes a small cut in your groin and inserts a thin, flexible tube (catheter) through an artery. This catheter is pushed until it reaches the renal artery. Contrast medium is injected through the tube, so that the renal artery is seen better on X-ray.
Other tests may also be done to check how well your kidneys are working. These tests include:
- Serum creatinine and blood urea nitrogen: Creatinine and urea are waste products removed from the body by your kidneys. Levels that are higher than normal mean your kidneys are damaged.
- Urinalysis: This test is used to check the physical and chemical properties of urine. Certain results may indicate kidney damage.
How is renal hypertension treated?
When you have renal hypertension, different treatment options may be available to help control your blood pressure and relieve narrowing of your renal arteries. These can also help prevent new or additional kidney damage. The treatment options include:
Medications
Your doctor may prescribe antihypertensive medications to help lower your blood pressure. There are many classes of antihypertensive medications, but 2 of the most effective ones are angiotensin-converting enzyme (ACE) inhibitors and angiotensin receptor blockers (ARBs).
ACE inhibitors and ARBs are rarely prescribed at the same time. They are also not given to people with narrowing or blockage of renal arteries on both sides because it can lead to worsening of kidney function.
Other medications that can be prescribed include calcium channel blockers (CCBs) and diuretics—medications that help the kidneys pass more fluid into the urine.
Angioplasty with stenting
Here, your doctor makes a small cut in your groin and inserts a catheter into an artery. The catheter carries a small inflatable balloon. When it reaches the blocked or narrowed area in the renal artery, the balloon is inflated, flattening the plaque and widening the vessel.
A tiny tube-like mesh (stent) can also be inserted by the catheter and left in place to support the previously narrow area of your artery.
Renal bypass surgery
This rare procedure may be done if your blood pressure and renal artery stenosis is not improved by antihypertensive medication and/or angioplasty. The surgeon creates an alternative route for blood flow by using a vein or synthetic tube to connect your kidney to your aorta.
What are the complications of renal hypertension?
With renal hypertension, uncontrolled high blood pressure can cause serious complications like:
- Stroke
- Heart attack
- Kidney failure
- Vascular dementia
- Retinopathy, a condition affecting the light-sensitive layer at the back of each eye.
- Excess fluid in the lungs (pulmonary edema)
- Thickening of the left pumping chamber of the heart (left ventricular hypertrophy)
- Heart failure
How can I prevent renal hypertension?
You may not be able to change certain factors that contribute to developing hypertension, but you can take steps to influence the factors within your control. Sticking to certain healthy habits can help you prevent renal hypertension while also helping to control your high blood pressure, if you already have the condition. The habits include:
- Regular exercise
- Reducing your weight, if you are overweight or obese
- Avoiding or stopping smoking
- Stopping or reducing your alcohol intake
- Reducing your caffeine intake
- Eating a DASH diet rich in vegetables, fruits, and whole grains while being low in sodium and cholesterol
What should I remember?
Renal hypertension, or high blood pressure caused by kidney issues, can lead to serious health problems, including heart disease, stroke, and kidney failure. When blood flow to the kidneys is restricted, the body reacts by raising blood pressure, creating a cycle that can worsen kidney damage over time.
Along with lifestyle changes and medications, regular blood pressure monitoring and kidney function tests are essential for those at risk. Awareness of symptoms, such as fatigue, swelling, or shortness of breath, can help with early detection. By understanding and managing renal hypertension, individuals can help protect their kidneys and overall health.