Hypertensive kidney disease is a condition where long-standing high blood pressure slowly damages the kidneys.
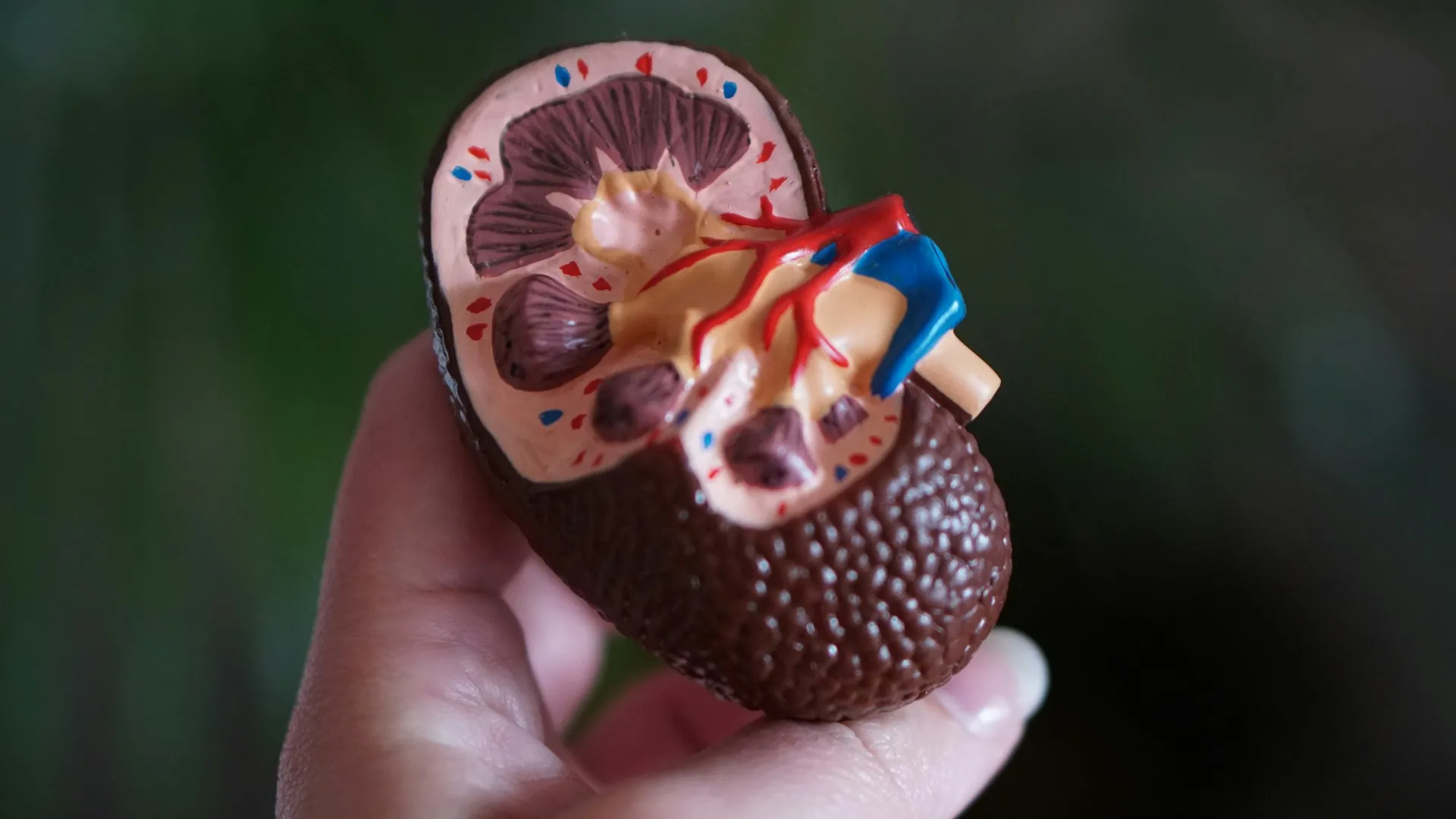
The kidneys are two bean-shaped organs located in the back of your abdomen on either side of your spine, just below the rib cage. They keep you healthy by:
- Filtering out waste products, excess water and toxins from the body.
- Making vitamin D, which is important for bone health.
- Maintaining normal levels of essential minerals in the body.
- Releasing erythropoietin, a hormone which tells your bone marrow to make red blood cells.
- Regulating blood pressure.
To perform these functions properly, each kidney has a network of many blood vessels within it. If these blood vessels are damaged by high blood pressure, your kidneys can start to malfunction.
About 1.3 billion adults aged 30–79 years worldwide have hypertension. About 1 in 10 people worldwide has chronic kidney disease; that is about 800 million people.
Hypertension is the second leading cause of chronic kidney disease after diabetes. In the United States, about 1 in 4 patients with end-stage kidney disease has hypertension.
Kidney disease can be both a cause and a result of high blood pressure. Renal hypertension is a type of high blood pressure caused by kidney disease.
How does high blood pressure cause kidney disease?
Blood pressure is the force which your blood applies on the walls of your arteries as it flows. According to the American College of Cardiology and American Heart Association guidelines, a person has high blood pressure (hypertension) when their blood pressure values are 130/80 mmHg or more.
High blood pressure can affect blood vessels throughout the body. In the kidneys, high blood pressure causes the blood vessels to become thick and stiff, therefore narrowing the vessel lumens (the hollow space through which blood flows). When this happens, the functional units in the kidneys, called nephrons, do not get enough oxygen and nutrients to do their work. So, wastes, toxins, and extra fluid build-up in the body.
The excess fluid can also increase the blood pressure further, creating a dangerous cycle. Worsening damage to the blood vessels may lead to kidney disease, and eventually kidney failure.
What are the symptoms of hypertensive kidney disease?
You may have hypertensive kidney disease and have no symptoms. As the condition worsens, you may start to notice progressive swelling of the feet, legs, hands, and face. Other symptoms of hypertensive kidney disease include:
- Nausea and vomiting
- Urinating more often, or less often
- Fatigue
- Muscle cramps
- Loss of appetite
- Numbness in the feet and hands
- Difficulty concentrating
- Trouble sleeping
- Shortness of breath
- Unintended weight loss
- Dry, itchy skin
Who is at risk of getting hypertensive kidney disease?
Anyone with high blood pressure can get hypertensive kidney disease. You may have higher chances of getting the condition if you:
- Have diabetes
- Are older than 65 years
- Are black
- Have poorly controlled moderate or severe hypertension
- Have a positive family history of kidney disease
- Have personal history of acute kidney injury
- Have certain genes
How is hypertensive kidney disease diagnosed?
If you have high blood pressure and symptoms of kidney disease, your doctor may suspect that you have hypertensive kidney disease. To diagnose your condition, a doctor will physically examine you. A healthcare provider will use an appropriate-size arm cuff to measure your blood pressure.
You may also have your heart examined using a stethoscope, and your eyes examined using a special instrument called a fundoscope. High blood pressure can affect many organs. So early identification and treatment of other hypertension-associated health problems, such as hypertensive retinopathy, can help you to live a better life. Evidence of hypertension-related damage to other organs can also be used to suggest hypertensive kidney disease.
Your doctor may also request that you have certain tests done to confirm the presence and severity of kidney damage. Some tests that may be done are:
- A blood test to check for the levels of creatinine, a waste product removed from the body by your kidneys. The levels of creatinine can also be used to estimate glomerular filtration rate (GFR), which is a measure of how well your kidneys are filtering blood. Kidney disease is associated with higher-than-normal blood creatinine levels and lower than normal GFR.
- A urine test to check for albumin. Albumin is a protein that is not filtered by healthy kidneys into urine. A high amount of albumin will be found in your urine if your kidneys are damaged.
- Kidney biopsy. This is where small samples of tissue are collected from your kidneys and examined under a microscope. If you have hypertensive kidney disease, the effect of high blood pressure on your kidneys will be observed by the pathologist.
What are the stages of hypertensive kidney disease?
There are 5 stages of any chronic kidney disease, including hypertensive kidney disease. Kidney disease staging depends on your GFR. GFR is expressed in milliliters per minute per 1.73 square meters of body surface area (mL/min/1.73 m2). The lower your GFR, the more advanced your kidney disease. The stages of hypertensive kidney disease are:
Stage | GFR |
1 | ≥ 90 |
2 | 60 – 89 |
3 | 30 – 60 |
4 | 15 – 29 |
5 | < 15 |
How is hypertensive kidney disease treated?
Hypertension-associated kidney damage cannot be reversed, but it is possible to prevent it or slow down its progression. The most important step is to manage the high blood pressure adequately. You will need to have a discussion with your doctor about your individual blood pressure targets, how to achieve them, and how often to measure your blood pressure.
Achieving and maintaining blood pressure targets usually requires a combination of medications and healthy lifestyle choices.
Medications
It is essential to adhere to the medications your doctor prescribes. Two essential types of blood pressure-lowering medications, angiotensin receptor blockers (ARBs) and angiotensin-converting enzyme (ACE) inhibitors, may also slow down progression of kidney disease.
You may need to take 2 or 3 different medicines to control your blood pressure. Other medications that may be added to an ACE inhibitors or ARB include:
- Diuretics (aka water pills) like furosemide, spironolactone
- Calcium channel blockers like nifedipine, amlodipine
- Beta-blockers like propranolol, bisoprolol
Lifestyle changes
Adjustments to your lifestyle that can help control your blood pressure include:
- Exercising regularly. Doing activities like cycling, swimming, jogging and brisk walking for at least 30 minutes a day, at least 5 days a week.
- Losing weight and maintaining a healthy weight. Talk to a healthcare professional about your weight goals and how to achieve them.
- Avoiding or quitting smoking.
- Eating a healthy diet. Because it can be difficult to follow a diet that is aimed at both reducing your blood pressure and slowing down kidney disease, you may need to talk to a dietitian to help you develop an appropriate meal plan.
- Taking steps to manage stress better. You may be able to manage stress adequately by engaging in physical activity, doing yoga, meditating, practicing helpful breathing exercises or listening to music that you like.
While taking steps to control your blood pressure, it will also be necessary to manage the kidney dysfunction. Depending on the results of certain blood tests, your doctor will prescribe necessary medications. If you have end-stage kidney disease, you may also need to have kidney transplantation or dialysis (where wastes, excess fluid and toxins are removed from the blood by methods not involving the kidneys).
How can I prevent hypertensive kidney disease?
When living with hypertension, you can protect your kidneys by ensuring that your blood pressure is well controlled. You need to take your medications as directed by your doctor. Because every patient is different, do not to take medications prescribed for someone else.
Healthy daily habits like exercising regularly, eating a balanced diet, maintaining a healthy weight, being well hydrated, and stopping smoking and alcohol intake can help you control your blood pressure and keep your kidneys healthy.
You also need to make sure other health conditions that can injure your kidneys are well managed. For example, you need to make sure kidney infections are treated promptly and that your blood sugar levels are well controlled, if you have diabetes.
What should I remember?
Hypertensive kidney disease is a serious condition where high blood pressure gradually damages the kidneys, reducing their ability to filter waste. Left untreated, it can lead to kidney failure and other severe health issues.
Protecting kidney health involves managing blood pressure through lifestyle changes, such as a balanced diet, reduced salt intake, regular exercise, and avoiding smoking and heavy alcohol use. Medications may also be necessary to keep blood pressure in check. Early detection and proper care can help slow kidney damage, allowing for a healthier and more fulfilling life.