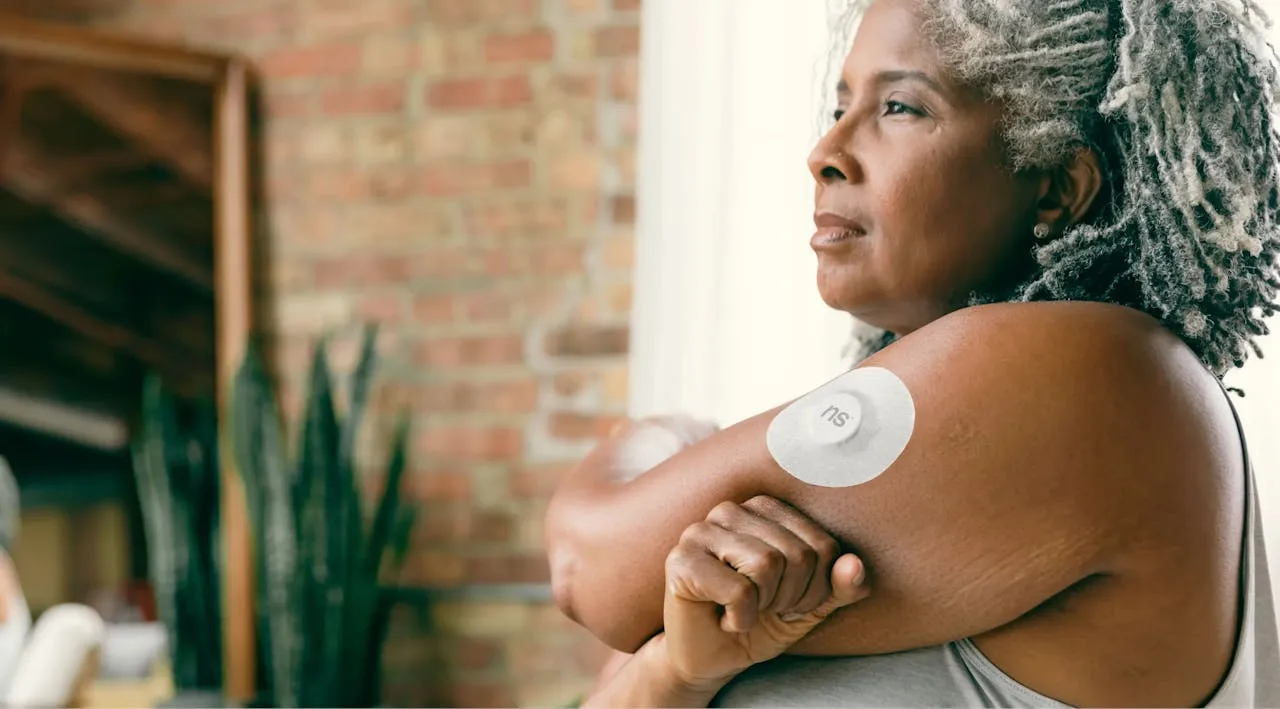
A continuous glucose monitor (CGM) is a device that automatically estimates your blood glucose (sugar) levels throughout the day and night.
CGM devices are mainly used by people with diabetes to closely monitor blood sugar levels and how they change throughout the course of the day in response to food intake, physical activity, medications, sleep, or other factors.
Because diabetes is a complex condition that can cause serious short-term and long-term health problems, regular monitoring and adequate control of blood sugar levels is essential for the health and well-being of all people living with the condition. Although usage of CGM devices is steadily increasing, finger stick measurements are still the most common single method used to monitor blood sugar.
How do CGMs work?
There are a number of CGM devices available on the market. Even though their makeup, appearance, and feel different, the way they function is remarkably similar. All CGMs share 3 basic parts. These are:
I. Sensor
This is a tiny piece of equipment, usually placed just under the skin of the abdomen or upper arm. An applicator makes the placement of a sensor quick, easy, and almost painless. The applicator has a needle which pierces the skin and allows the sensor to be inserted in the fat tissue under it. After insertion, the needle is withdrawn and sticky tape is used to keep the sensor in position.
The sensor can then start measuring glucose in the interstitial fluid, which the fluid between your cells. Interstitial fluid contains wastes from cells and substances that leak out of blood capillaries, including glucose.
Glucose levels in the interstitial fluid are very similar to those in the blood, but with a slight time lag between them. This is because glucose levels increase or decrease in the blood before the change is transmitted to the interstitial fluid.
Sensors also have a warm-up time, after which they start communicating with other components of the CGM. Warm-up time depends on the type of CGM and usually ranges from 30 minutes to 2 hours. After warm-up, some CGM devices require finger stick blood glucose calibration before sharing glucose data. Calibration is to ensure that CGM measurements are accurate enough. Calibration may need to be repeated at regular intervals.
II. Transmitter
The transmitter wirelessly sends information from the sensor to the device, where it can be viewed. Some transmitters are non-reusable and permanently attached to the sensor. Other transmitters are reusable and can be attached to a new sensor when an earlier one is disposed off.
III. Display device
Information from the transmitter can be viewed on a compatible insulin pump, smartphone, or a special device called a receiver (reader).
On these devices, you can see your current glucose levels, past glucose levels, and how fast your levels are falling or rising. You can also set your device to alert you when your sugar goes below or above a certain range of glucose levels.
How often should I change the sensor and transmitter of my CGM system?
Generally, there are 2 types of CGM sensors: disposable sensors and implantable sensors. Depending on the brand of CGM, disposable sensors need to be replaced every 7–15 days.
Implantable sensors are typically placed under the skin of the upper arm by a healthcare provider. They last much longer than disposable ones, usually a couple of months or longer. The Eversense E3 CGM sensor can last up to 6 months, while the Eversense 365 CGM sensor can last up to a year.
Transmitters that are part of a single sensor-transmitter device will be replaced as frequently as you change the sensor. Depending on the brand, reusable transmitters can last anywhere from 3 months to 5 years. Some reusable transmitters also require charging before they can be connected to the sensor.
What are the types of CGMs?
All CGM systems measure glucose levels continuously but can be classified depending on how they store and display glucose data. The 3 types of CGMs are:
- Real-time CGMs (rtCGMs): These measure glucose levels continuously and store and display glucose data automatically.
- Intermittently scanned CGMs (isCGMs): They are also called flash glucose monitors. They measure glucose levels continuously. But every few hours, they require scanning with a smartphone or receiver to display and store glucose data.
- Professional CGMs: They are placed on a patient by a healthcare professional. They are typically used by a doctor to monitor glucose levels and trends for a short period of time. Glucose data may, or may not, be available to the patients whose levels are being monitored.
Who can use a Continuous Glucose Monitor?
CGMs are usually recommended for people living with type 1 and type 2 diabetes. They can be used for short-term or long-term monitoring of blood sugar levels in diabetes patients who are 2 years or older.
CGMs may also be used in patients with other medical conditions that can affect blood glucose levels. These conditions include:
- Gestational diabetes
- Obesity
- Prediabetes
- Insulinoma—a rare tumor associated with hypoglycemia (low blood glucose) because of excessive insulin secretion.
What are the benefits of using CGMs when managing diabetes?
There are a number of advantages of choosing a CGM over a glucose meter (glucometer) as the main tool for keeping track of your glucose levels. CGM devices:
- Reduce the number of finger stick tests you need to do.
- Alert you when glucose levels rise above, or fall below a certain preset range. So, they help you to prevent or seek early treatment for episodes of low blood glucose or high blood glucose.
- Help your diabetes care team to manage your diabetes better. CGMs allow your team to make decisions based on extensive glucose data including how your glucose levels change in response to certain conditions like illness, stress, eating patterns, exercise, and medications.
- Reduce your chances of getting long-term diabetes complications.
What are the disadvantages of using CGMs?
Although CGMs are an important component of any diabetes care toolkit, they may also present some issues to deal with. Disadvantages of using CGMs include:
- High cost of CGM systems. Check with your healthcare insurance provider to confirm how much of your CGM device and supplies are covered by your plan.
- It may be uncomfortable to have them on, especially when you have just started using them.
- They may contribute to diabetes-related stress and anxiety. This can be due to providing more glucose information than is necessary (information overload), fear of device malfunction, or getting too many warning alerts (alarm fatigue).
- It may take some time to properly learn how to use them. You will need to learn how to set device alarms, interpret readings, troubleshoot problems, insert and replace sensors and transmitters.
- Skin irritation from the sticky tape used to hold the device in place. This can cause itching, redness, bruising, rash, or scarring. Talk to a doctor to help you prevent or treat skin issues.
What can affect the accuracy of CGM measurements?
Accuracy may differ amongst brands and models of CGM devices. But with proper use, most CGM measurements can be as accurate as finger stick readings. Factors that can affect the accuracy of CGM measurements include:
I. Pressure
Pressing on tissue around the CGM sensor can decrease blood flow to it and cause falsely low glucose values. This is called compression hypoglycemia or compression artifact. Removing pressure on the sensor rapidly normalizes glucose values.
II. Calibration issues
For devices that require calibration with finger stick glucose measurement, make sure you do so as often as is necessary. Wash your hands thoroughly and dry them before the finger stick test. Also, calibrate when blood glucose is stable, usually in the mornings or before bed.
III. Sensor issues
New sensors may be inaccurate in the first 24 hours after inserting them. This is a calibration period during which the sensor gradually becomes more accurate. Keeping a sensor longer than is recommended can also cause inaccurate measurements. Make sure you replace your disposable sensor according to the device instructions.
IV. Medications
Depending on the brand of CGM, certain medications and supplements can affect how well the sensor measures glucose levels. These include:
- Acetaminophen (Paracetamol)
- Aspirin
- Tetracycline
- Ascorbic acid (vitamin C)
- Mannitol—a medication used to treat increased pressure within the skull
- Hydroxyurea—a medication mainly used to manage sickle cell disease
Discuss with your doctor if you have to take these medications while using a CGM.
What should I remember?
Continuous glucose monitors (CGMs) offer real-time insights into blood sugar levels, helping people make better decisions about their diet, exercise, and medication. By reducing the need for frequent finger pricks, CGMs provide a more convenient way to monitor glucose.
While CGMs improve glucose control, they have some limitations like cost, alarm fatigue, information overload, and occasional inaccuracies.
If you’re living with diabetes, a CGM could make life easier and improve your health. Talk to your doctor to see if a CGM is right for you. With the right tools and guidance, managing diabetes can become more effective and less overwhelming.